Signs & symptoms of Dermatomyositis in adults & children
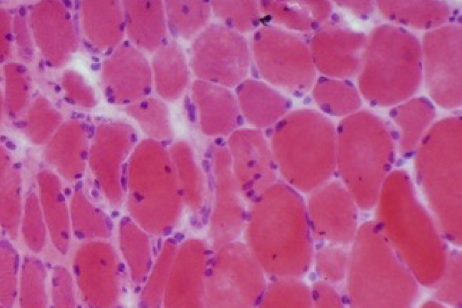
Common characteristics of dermatomyositis in adults and children include proximal muscle weakness, muscle inflammation and a characteristic skin rash.1,2
Onset of dermatomyositis may be acute or insidious, and the rash may accompany or, more commonly, precede the onset of muscle weakness.1-3
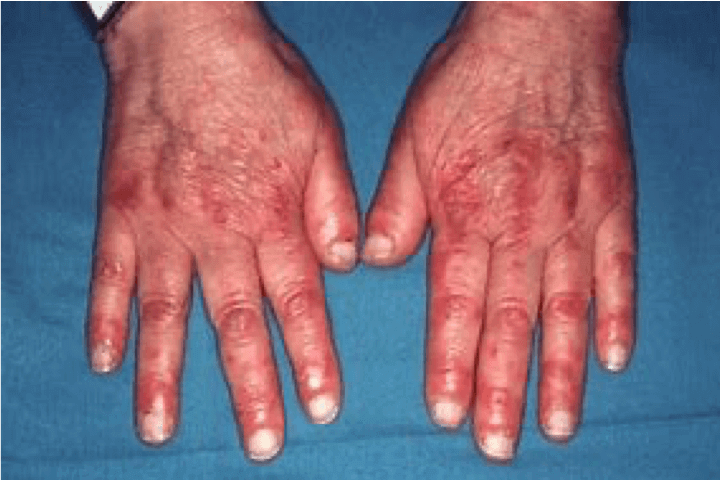
The rash commonly occurs in photosensitive areas and is erythematous, oedematous and occasionally pruritic.1
Skin and muscle involvement1,2
The skin and muscle involvement in dermatomyositis can vary from person to person, but common features may include:
Pathognomonic heliotrope rash

- Red discoloration over the upper eyelids, with or without periorbital oedema
- Malar and facial rash
Shawl sign
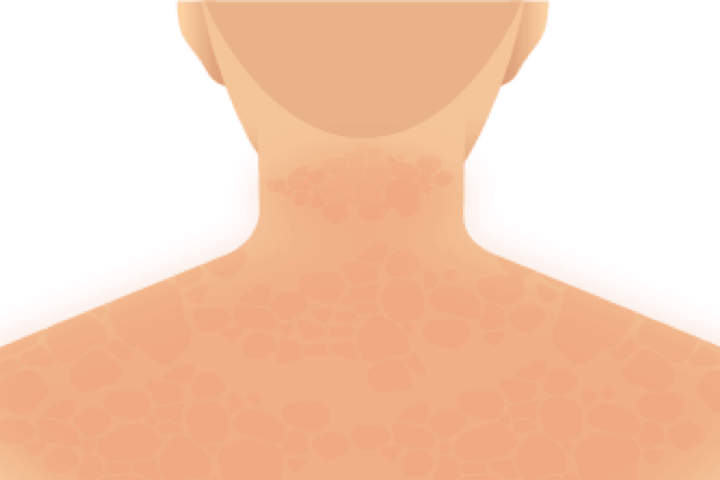
- Rash on neck, back and shoulders
V-sign
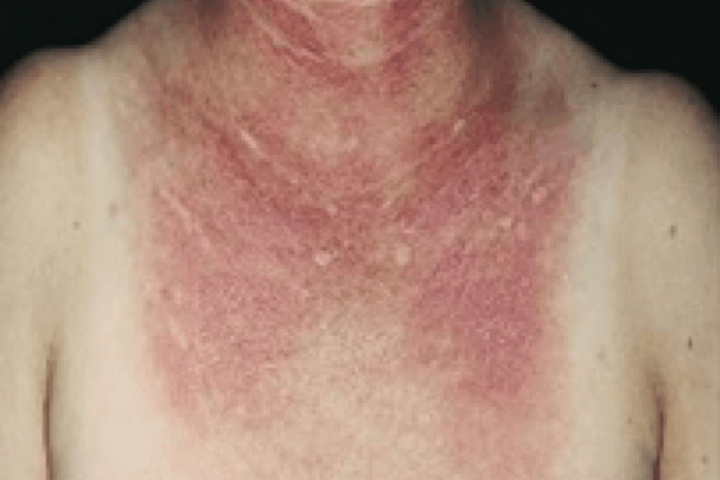
- Rash on anterior chest
Gottron's sign
Juvenile dermatomyositis is characterised by insidious onset of weakness and myalgia following a fever, fatigue or skin rash.1 Patients exhibit irritability and a reluctance to socialise.3 Complications include calcinosis cutis (subcutaneous calcifications), and vasculopathy affecting the gastrointestinal tract.2
Calcinosis cutis is more common in juvenile than adult dermatomyositis.1 Its presence suggests active disease and may be associated with diagnostic and treatment delay.2
Although dermatomyositis is usually painless, pain can be significant in patients with acute disease and calcinosis cutis.2

Common characteristics of dermatomyositis include proximal muscle weakness, muscle inflammation and a characteristic skin rash.3
The image shows the V-sign rash, a characteristic skin finding in people with dermatomyositis. The V-sign rash is a purplish or reddish rash that appears on the anterior chest in a V-shaped pattern. It may be accompanied by scaling and is often one of the first signs of dermatomyositis.3
Other complications in dermatomyositis
Other complications in dermatomyositis include malignancy and conditions affecting the joints or the pulmonary, cardiac and gastrointestinal systems.1,2
Systemic complications create challenges for clinicians as patients often have concurrent severe muscle weakness, skin rashes and life-threatening organ involvement, making disease management and treatment more complicated.4
The list below shows information about other complications in dermatomyositis besides muscle weakness and skin involvement:
Cardiac
- While most dermatomyositis patients do not develop cardiac symptoms, arrhythmias or defects in ejection fraction may be present due to involvement of the cardiac muscle in dermatomyositis1
- Pericarditis, myocarditis and congestive heart failure, despite being rare in dermatomyositis, may lead to increased mortality1
Pulmonary
- Interstitial lung disease (ILD) is a common pulmonary manifestation of dermatomyositis9
- ILD manifests as a non-productive cough and dyspnoea, and is the leading cause of death in dermatomyositis patients1
- Survival is significantly worse for dermatomyositis patients with ILD compared with those without (p=0.02)10
- DM is also associated with weakness of the ventilatory muscles2
- There is a strong association between ILD development and MDA-5 autoantibodies11
Gastrointestinal
Malignancy
- Risk of malignancy is increased in patients with adult-onset dermatomyositis1,5,6
- A meta-analysis found that patients with dermatomyositis had a 5.5-fold higher risk for malignancy compared with the general population7
- Cancers commonly associated with dermatomyositis include ovarian, breast, colon, nasopharyngeal (Asian populations), melanoma, and non-Hodgkin’s lymphoma8
- Certain autoantibody subtypes are associated with increased risk of malignancy, and these patients should be investigated for malignancies and closely monitored1
Joints
- Large-joint and small-joint arthralgia are common in dermatomyositis with or without an underlying arthritis1
Learn more about the diagnosis of Dermatomyositis
References
- Goyal, N. A. (2019). Immune-Mediated Myopathies. CONTINUUM: Lifelong Learning in Neurology, 25(6), 1564–1585. https://doi.org/10.1212/con.0000000000000789
- Malik, A., Hayat, G., Kalia, J. S., & Guzman, M. A. (2016). Idiopathic Inflammatory Myopathies: Clinical Approach and Management. Frontiers in Neurology, 7. https://doi.org/10.3389/fneur.2016.00064
- Dalakas, M. C., & Hohlfeld, R. (2003). Polymyositis and dermatomyositis. The Lancet, 362(9388), 971–982. https://doi.org/10.1016/s0140-6736(03)14368-1
- Oddis, C., & Aggarwal, R. (2018). Treatment in myositis. Nature Reviews Rheumatology. https://doi.org/10.1038/nrrheum.2018.42
- Chen et al., Cancer risks of dermatomyositis and polymyositis: a nationwide cohort study in Taiwan Arthritis Research & Therapy 2010, 12:R70. doi: 10.1186/ar2987
- Airio, A., Kautiainen, H., & Hakala, M. (2006). Prognosis and mortality of polymyositis and dermatomyositis patients. Clinical Rheumatology, 25(2), 234–239. https://doi.org/10.1007/s10067-005-1164-z
- Yang, Z., Lin, F., Qin, B., Liang, Y. and Zhong, R. (2014). Polymyositis/dermatomyositis and Malignancy Risk: A Metaanalysis Study. The Journal of Rheumatology, 42(2), pp.282–291. doi:https://doi.org/10.3899/jrheum.140566.
- Dalakas, M.C. (2015). Inflammatory Muscle Diseases. New England Journal of Medicine, 372(18), pp.1734–1747. doi:https://doi.org/10.1056/nejmra1402225.
- Morisset, J., Johnson, C., Rich, E., Collard, H. R., & Lee, J. S. (2016). Management of Myositis-Related Interstitial Lung Disease. Chest, 150(5), 1118–1128. https://doi.org/10.1016/j.chest.2016.04.007
- Dankó, K., Ponyi, A., Constantin, T., Borgulya, G., & Szegedi, G. (2004). Long-term survival of patients with idiopathic inflammatory myopathies according to clinical features: a longitudinal study of 162 cases. Medicine, 83(1), 35–42. https://doi.org/10.1097/01.md.0000109755.65914.5e
- Sato, S., Murakami, A., Kuwajima, A., Takehara, K., Mimori, T., Kawakami, A., Mishima, M., Suda, T., Seishima, M., Fujimoto, M. and Kuwana, M. (2016). Clinical Utility of an Enzyme-Linked Immunosorbent Assay for Detecting Anti-Melanoma Differentiation-Associated Gene 5 Autoantibodies.PLOS ONE, 11(4), p.e0154285. doi:https://doi.org/10.1371/journal.pone.0154285.
Science Hub
Sign up and connect to Science Hub to learn more about our recent ProDERM study and have access to symposia presentations, publications, posters and lectures.